Soon after I met Melissa, we both knew—in true lesbian fashion—that we wanted to get married and have a baby. We didn’t know if either would be possible, or how long we’d have to wait. It turned out to be five years and fifteen years, respectively.
Once the decision to have a baby is made, the questions that follow might be: When? And how many? For many couples, the questions end there. For us, they continued: Who is going to carry? Will we both try? Who first? What method? And with what sperm? Should we go to a sperm bank or use a known donor? If a known donor, who? What method should we start with? Can we afford it? What will insurance cover?

I called member services at our insurance company to find out if any fertility services were covered. “Have you been trying consistently for at least a year?” they asked me. This was after I told them my wife and I were trying to conceive. As a lesbian couple, our reproductive situation didn’t correspond with the medical system’s narrative; we both had the ability to conceive and carry a child, and—as far as we knew when we started—we didn’t have any issues with fertility. We were just missing one key component: sperm. Clearly, the health care system was behind. Once, we were given an after-visit summary that suggested we “continue to have intercourse several times during your ovulation window.” If only it was that easy.
We decided I would try to conceive first because I’m six years older, and that we would try at home with donations from a known donor, the method that was most “natural,” even though it felt anything but.
When we decided to use a known donor, we learned about the byzantine process required to use that sperm for insemination: The sperm has to clear FDA regulations for tissue donation; a legal agreement must be in place; the donor needs to pass medical and sexual history screenings, physical exams, infectious disease testing, and a psychological exam; the recipients, separately and jointly with the donor, must pass a psychological exam; frozen sperm samples must be quarantined for three to six months; finally, the frozen sample must be thawed and retested before final release.
After several unsuccessful at-home inseminations, I had fertility tests done. I had low ovarian reserve, and my egg quality was not great. A doctor tried to reassure me, but I couldn’t help but picture chicken eggs inside me, brittle and mottled, hairline fractures threatening a few.
We tried over and over, sometimes both of us at the same time. We tried at home, in a medical office, at our donor’s home, at a friend’s home. Both of us got pregnant multiple times, but neither of us could sustain a pregnancy. Unexplained infertility, we were told.
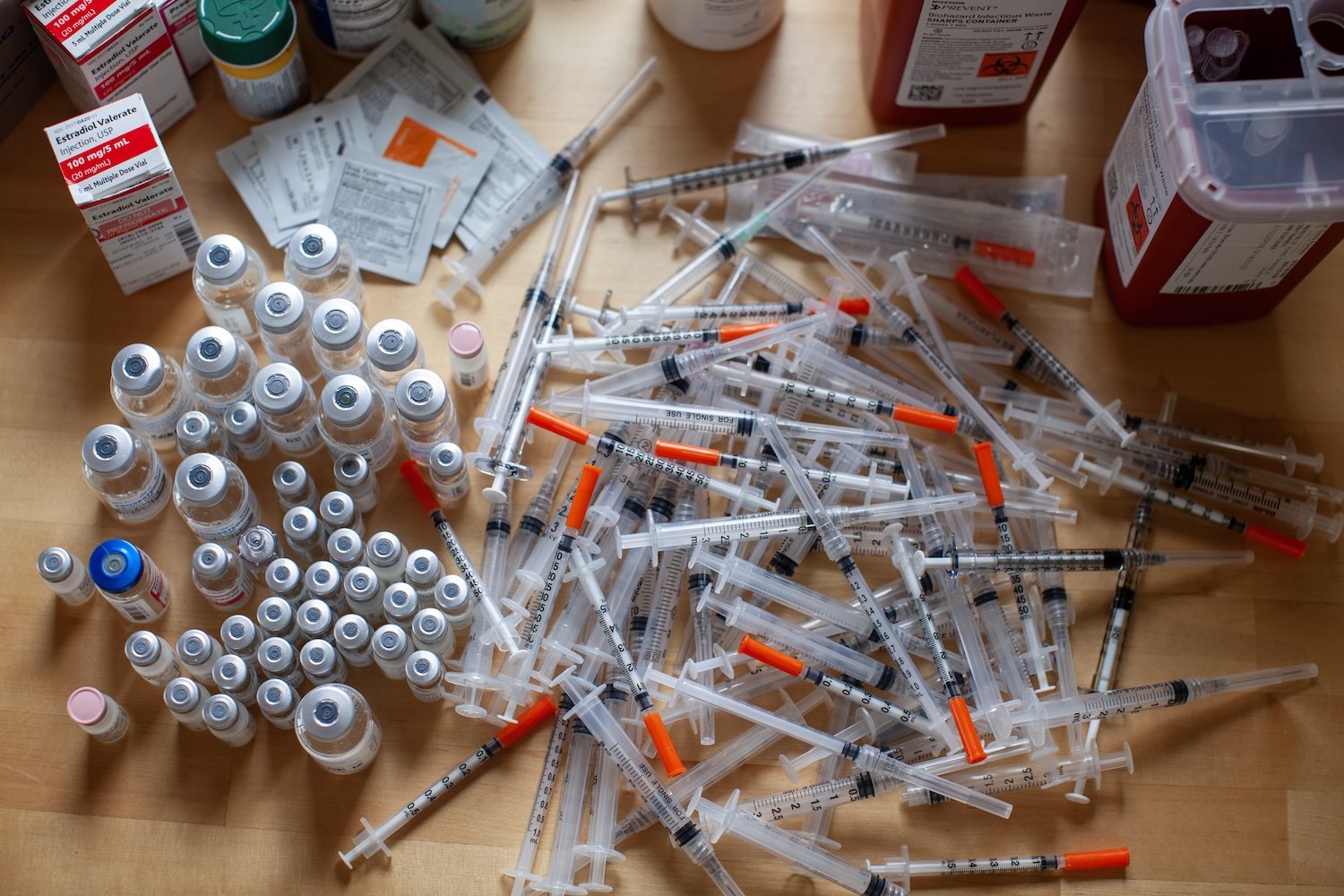
After seven years of attempting to conceive through methods that entail less medical intervention, we decided to try in vitro fertilization, or IVF. We knew it would be an involved process, but we didn’t realize how much it takes over your life. There are shots. Many, many shots. And they have to be administered at the same time every day. We received boxes of medication, some of which needed to be refrigerated. We fashioned an old shoebox into a portable medical bay replete with alcohol wipes, needles of various sizes, syringes, and vials of liquid hormones.
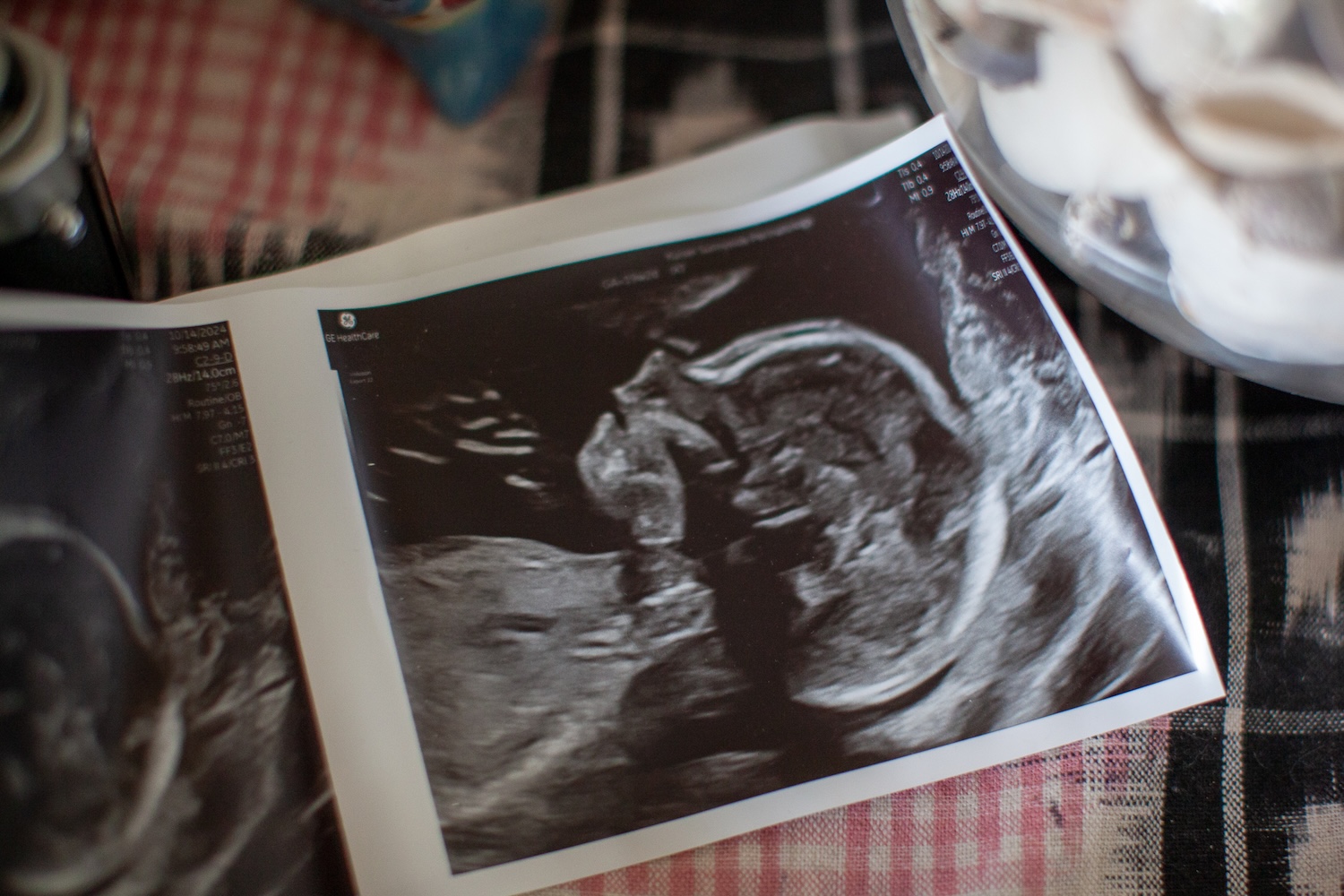
For someone who doesn’t like needles, has fainted multiple times in doctor’s offices, and didn’t excel in chemistry, this was going to be a challenge. We ordered an auto-injector from Denmark and learned new terms like Luer lock. I felt like a chemist: mixing, measuring, prepping, injecting. It felt vaguely illegal—or like we should have had more training. What if I hit a nerve? Or a blood vessel? Somehow, Queen Latifah became our soundtrack for injections. Not her seminal album Black Reign or her debut, All Hail the Queen, but inexplicably, her cover of “Walk the Dinosaur” from the movie Ice Age: Dawn of the Dinosaurs. I haven’t listened to it since.

Other memories still come back to me in flashes: buying a comically large blue plastic soup bowl at Walgreens when we realized we had no container for our impending donor sample; seat-belting a large cardboard box containing a liquid nitrogen tank with our donor sperm in it into the passenger seat of my car; holding a small jar of sperm between my legs to keep it warm in the Nebraska winter; my wife’s pained face during a dilation and curettage procedure where she wasn’t properly anesthetized; realizing I was miscarrying while eating tacos on Northeast Alberta Street.

Despite the flashes, most of the details of this time are lost to me. Did my brain bury them because the emotional weight was too much to bear? Or maybe, once our baby was born, a kind of blissful postpartum amnesia took hold, the elation of finally having a child sanding off the most jagged edges of the pain. Maybe our path seems less treacherous and depressing when you know that at the end of it lay what we always wanted: a baby.

Comments
No comments yet.
Add a Comment